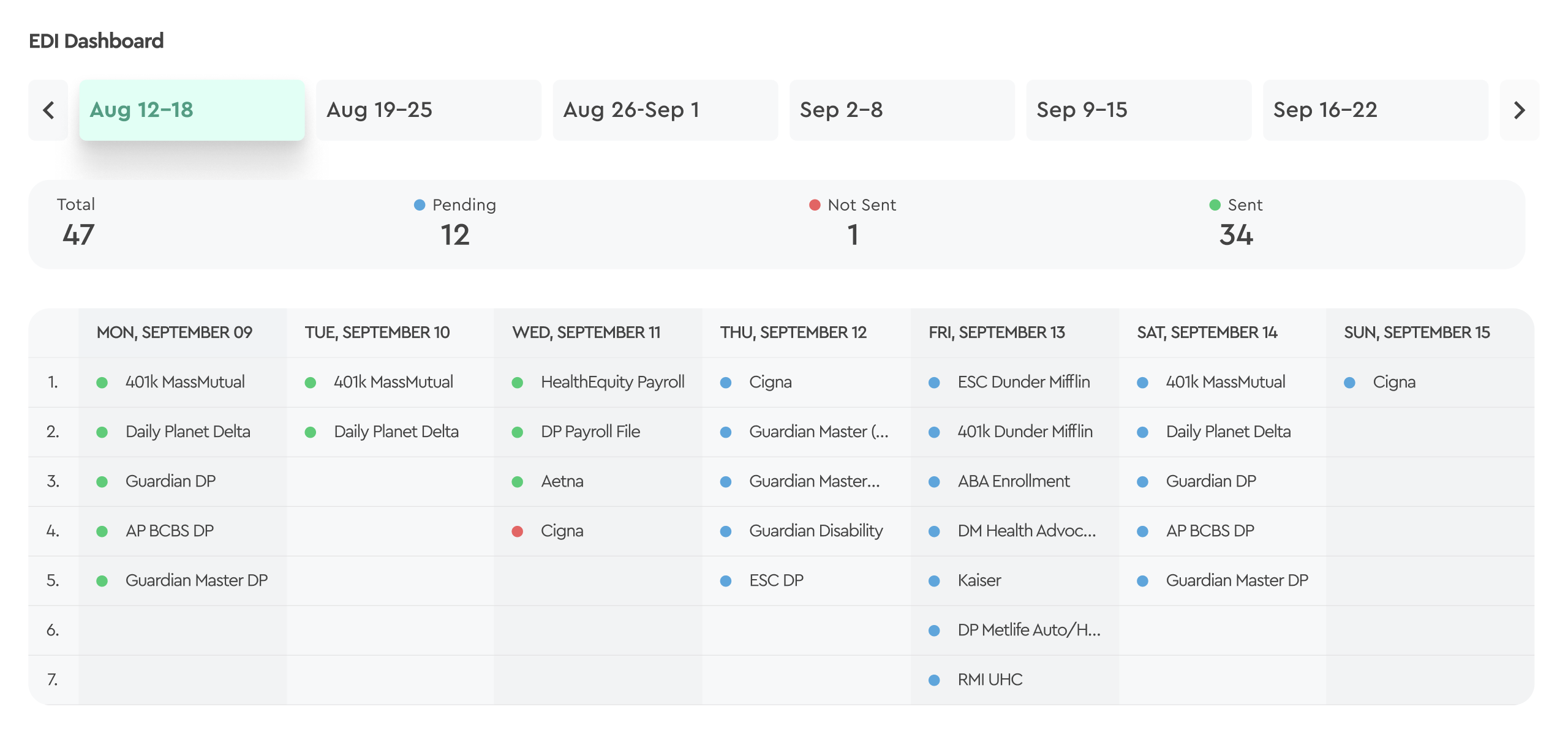
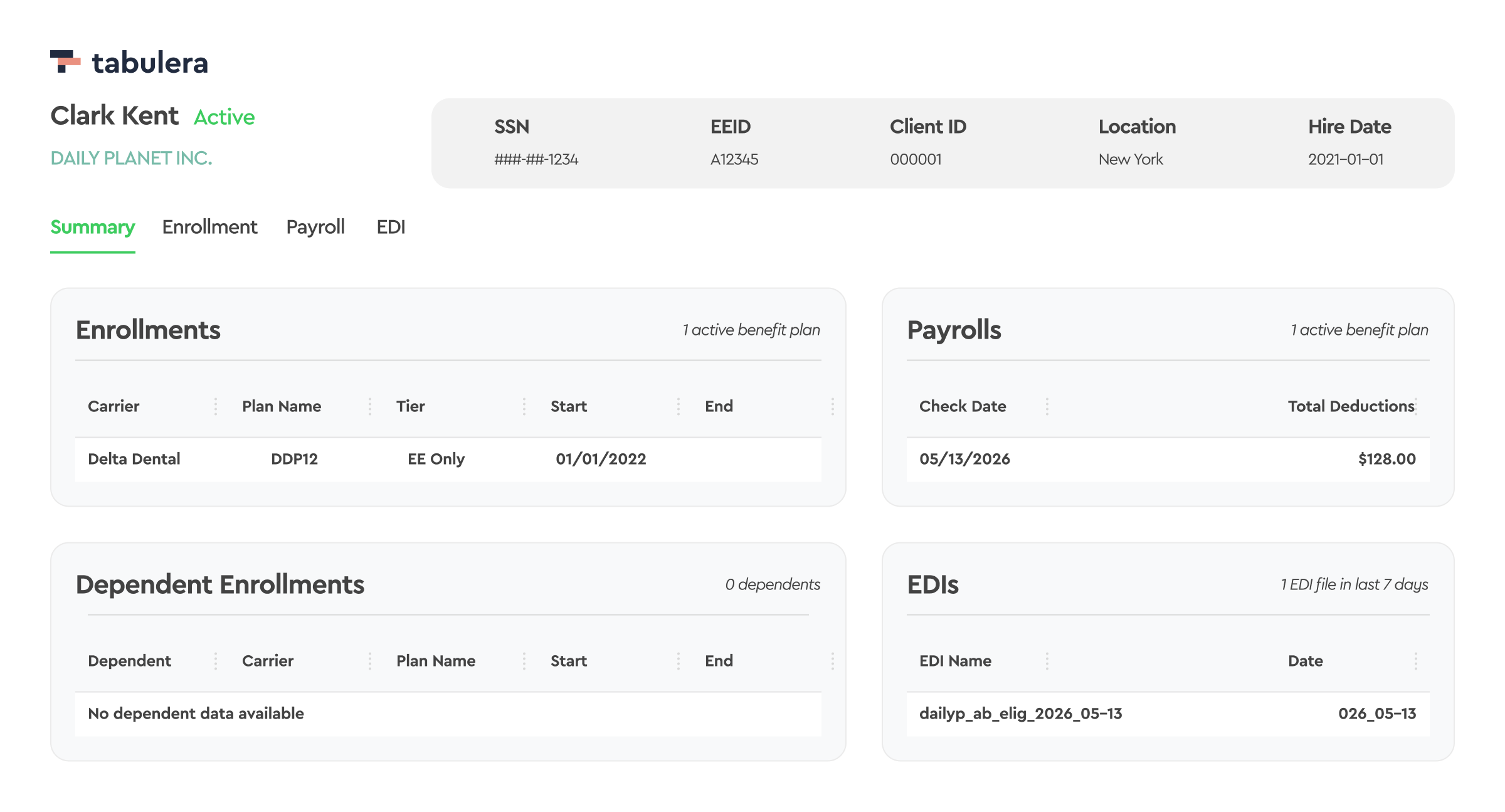
Yes. Our EDI 834 solution connects with platforms like PrismHR, isolved, Employee Navigator, and Workday — no migration or platform changes required.
EDI 834 Service Provider – Go Live in 30 Days
Fastest EDI Benefits Carrier Integration
Tabulera is a white-glove EDI 834 service provider combining expert execution and full-visibility software, delivered in 30 days.
Providing EDI Services to world best teams